How SLSA and SBOM can help healthcare's cybersecurity resiliency

Taylor Lehmann
Director, Office of the CISO
Seth Rosenblatt
Security Editor, Google Cloud
Taking prescription medication at the direction of anyone other than a trained physician is very risky—and the same could be said for selecting technology used to run a hospital, to manage a drug manufacturing facility and, increasingly, to treat a patient for a medical condition.
To pick the right medication, physicians need to carefully consider its ingredients, the therapeutic value they collectively provide, and the patient’s condition. Healthcare cybersecurity leaders similarly need to know what goes into the technology their organization's use to manage patient medical records, manufacture compound drugs, and treat patients in order to keep them safe from cybersecurity threats.
Just like prescription medication, careful vetting and selection of the technology is required to ensure patient safety and establish visibility and awareness into the technology modern healthcare depends on to create a resilient healthcare system.
In this and our next blog, we focus on two topics critical to building resilience - software bill of materials (SBOM) and Google’s Supply chain Levels for Software Artifacts (SLSA) framework - and how to use them to make technology safe. Securing the software supply chain, or where the software we depend comes from, is a critical security priority for defenders and something Google is committed to helping organizations do.
Diving deeper into the technology we rely on
Cybersecurity priorities for securing healthcare systems usually focus only on protecting sensitive healthcare information, like Protected Health Information (PHI). Maintaining the privacy of patient records is an important objective and securing data and systems plays a big role in this regard.
Healthcare system leadership and other decision makers often depend on cybersecurity experts to select technologies and service providers that can meet regulatory rules for protecting data as a first (and sometimes only) priority. Trust is often placed on the reputations and compliance programs of the vendors who manufacture the technology they buy without much further inspection. Decision makers need to approach every key healthcare and life science technology or service provider choice as a high-risk, high-consequence decision, but few healthcare organizations have the skills, resources, and time to “go deep” in vetting the security built into the technology they buy before it enters a care setting.
Vetting needs to include penetrating analysis of all aspects of software and hardware, their architecture and engineering quality, the provenance of all parts that they’re made of, and assessing each component for risk. Doing this can sometimes require deep technical skills and advanced knowledge of medical equipment threats that may not be easy to acquire. Instead of making additional investments to help secure their networks and systems, many organizations choose simpler paths.
The failure to properly assess technological susceptibility to risk has exposed healthcare organizations and their patients to a variety of safety and security issues that may have been preventable. PTC (formerly Parametric Technology Corporation, which makes medical device software) disclosed seven vulnerabilities in March that impacted equipment used for robotic radiosurgery. In October 2019, the VxWorks Urgent 11 series of vulnerabilities was announced, affecting more than 1 billion connected devices, many used throughout healthcare and life sciences. More examples of medical devices and software found to have vulnerable components can be found on the FDAs cybersecurity website and in its recall database.
How a physician understands, selects, and prescribes medication parallels how we address these concerns when selecting technology. Recent FDA guidance suggests manufacturers must soon provide increased levels of visibility into the technologies they market and sell in the healthcare industry. Here’s where the SBOM, a key visibility mechanism, comes in.
What SBOMs do well, and how Google is helping make them better
The National Telecommunications and Information Administration defines the SBOM as a “nested inventory for software, a list of ingredients that make up software components.”
The concept of a SBOM appears to have found its start in enabling software makers back in the 1990s, although it originally stems from ideas popularized by visionary engineer and professor W. Edwards Deming. SBOM as a concept has advanced since then, with multiple standards for generating and sharing them now in use.
Thanks to the continued focus on improving and using SBOMs, we expect it will be much easier for defenders to use SBOMs to track software and its components, where they come from, what security vulnerabilities they contain, and equip protectors with their ability to stop those vulnerabilities from being exploited, at scale, and before they impact patient care.
“Software bills of materials help to bridge the knowledge gap created by running unknown, unpatched software and components as too many healthcare organizations currently do,” says Dan Walsh, chief information security officer at VillageMD, a tech-driven primary-care provider. “For security leaders, SBOM should be an extension of their asset inventory and management capability, regardless of whether that software was bought or built. At VillageMD, we are asking our vendors that store, transmit, receive or process PHI for an SBOM as part of our third-party vendor assessment program.”
Today’s SBOMs are most often basic text files generated by a software developer when the creation of software is complete and a product is assembled (or application is created from source code.) The text file contains information about the product’s software components and subcomponents, where those components and subcomponents came from, and who owns them. But unlike a recipe used to make a pharmaceutical, for example, an SBOM also tracks the software versions of components and subcomponents. SBOMs often capture:
- Supplier Name
- Component Name
- Version of the Component
- Other Unique Identifiers
- Dependency Relationship
- Author of SBOM Data
- Timestamp
Here’s the format of a SBOM generated using the SPDX v2.2.1 standard:
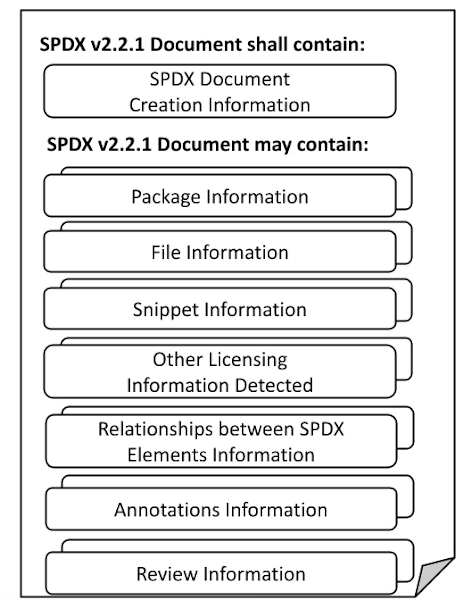

Technology producers, decision makers, and operators in any industry can use this information to deeply understand the risks the products pose to patients and the health system. An SBOM, for example, can show a reader if the software used on a medical device is merely out of date, or vulnerable to a cyber attack that could affect its safe use.
Google sponsors a number of initiatives focused on securing the software supply chain, including how to use SBOMs, through our work with U.S. government agencies, the Open Source Security Foundation, and Linux Foundation, including a project focused on building and distributing SBOMs. Learn about the SPDX project and Cyclone DX, read the ISO/IEC 5962:2021 standard (for SPDX), ISO ISO/IEC 19770-2:2015 (for SWID; another artifact that provides a SBOM), and other training resources from the Linux Foundation.
As an additional measure, healthcare organizations which use SBOM need to make sure they can trust that the SBOMs they rely on haven’t been changed since the manufacturer produced it. To defend against this, software makers can cryptographically sign their SBOMs making it easier to identify if a SBOM has been maliciously altered since it was first published.
While U.S. Executive Order 14028 created a federal mandate for the SBOM, and although many organizations have begun to incorporate that mandate into their software production workflows, many issues and roadblocks remain unresolved. At Google, we think the use of SBOM will help organization's gain important visibility into the technologies that are entering our healthcare facilities and enable defenders to more capably protect both patient safety and patient data privacy.
Digging into the SLSA
We believe resilient organizations have resilient software supply chains. Sadly no single mechanism, like SBOM, can achieve this outcome. It’s why we created the SLSA framework, and services like Assured Open Source Software. SLSA was developed following Google’s own practices for securing its software supply chain.
SLSA is guidance for securing software supply chains using a set of incremental, enforceable security guidelines that can automatically create auditable metadata. This metadata will then result in a "SLSA certification" to a particular package or build platform. It’s a verifiable way to assure consumers that the software they use hasn’t been tampered with, something which doesn’t exist broadly today. We’ve recently explained more about how the SLSA works in blog posts on SLSA basics and more in-depth SLSA details.
Similarly, Assured Open Source Software gives organizations the ability to use the same regularly tested and secured software packages Google uses to build its software. Used in combination with a SBOM, technology makers can build reliable, safe, and verifiable products. Most technology buyers, such as those who run your local healthcare system, can use those same mechanisms to gain visibility into a technologies’ safety and fitness for use.
Where do we go from here?
Visibility into the components that make up the technology we use to care for patients is critically necessary. We can’t build a resilient healthcare system if our only priority is privacy of data. We must add resilience and safety to the list of our top priorities. Gaining deep visibility into the technology that decorates health system networks is a critical shift we must make. SBOM and SLSA help us make this shift. But remember, it’s not one or the other. As Dan Walsh from VillageMD says, the SBOM has a way to go:.
“It won't solve all of your problems,” he cautions, but adds that when used correctly, “SBOM will help you improve visibility into the software that runs on the critical systems that keep societies safe and we're excited to see it get traction.”
But when complemented with SLSA and topics we’ll cover next, such as a Vulnerability eXploitability Exchange (VEX), we are on a path to greater resilience.


